ROS1 fusions in Chinese patients with non-small-cell lung cancer
Background
To determine the prevalence and clinicopathological features of ROS1 fusions in Chinese patients with non-small-cell lung cancer (NSCLC).
Methods
Formalin-fixed and paraffin-embedded (FFPE) tissue sections from 392 patients with NSCLC were screened for ROS1 fusions by multiplex RT–PCR and all ROS1 fusions were validated by direct sequencing. The relationship between ROS1 fusions and clinicopathological features and the prognostic effect of the ROS1 fusion status on survival were analyzed.
Result
In this study, 8 of 392 (2.0%) evaluable samples were found to harbor ROS1 fusions. Of the ROS1-positive patients, seven presented with adenocarcinoma, and one with adenosquamous carcinoma. The ratio of female to male and never smoker to smokers in a ROS1 fusion-positive group was 5:3. There was no statistically significant difference in age, sex, smoking history, histological type and pathological stage between ROS1 fusion-positive and ROS1 fusionnegative patients. ROS1 fusion-negative patients had a significantly longer survival when compared with ROS1 fusionpositive patients (P = 0.041). Lower pathological stage, younger age and ROS1 fusion-negative status were significantly associated with better prognosis on multivariate analysis.
Conclusion
ROS1 fusions occurred in ∼2.0% of Chinese patients with NSCLC and had no specific clinicopathological feature. ROS1 fusion-negative patients may have a better survival than ROS1 fusion-positive patients.
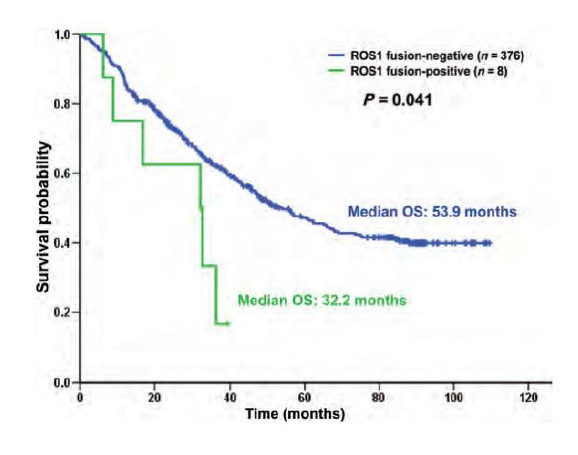
Figure. The comparison of overall suvival between ROS1-negative and ROS1-positive patients using theKaplan–Meier method.


